Topical Steroid Risk Calculator
Calculate Your Risk
Low Risk
Your usage pattern shows minimal risk of skin atrophy and infections.
Using topical corticosteroids for eczema, psoriasis, or rashes can bring quick relief-but what happens when the relief lasts too long? Many people don’t realize that even short-term use of strong steroid creams can silently damage the skin, leading to thinning, infections, and a painful withdrawal process that can last months. This isn’t rare. It’s common. And it’s often missed until it’s too late.
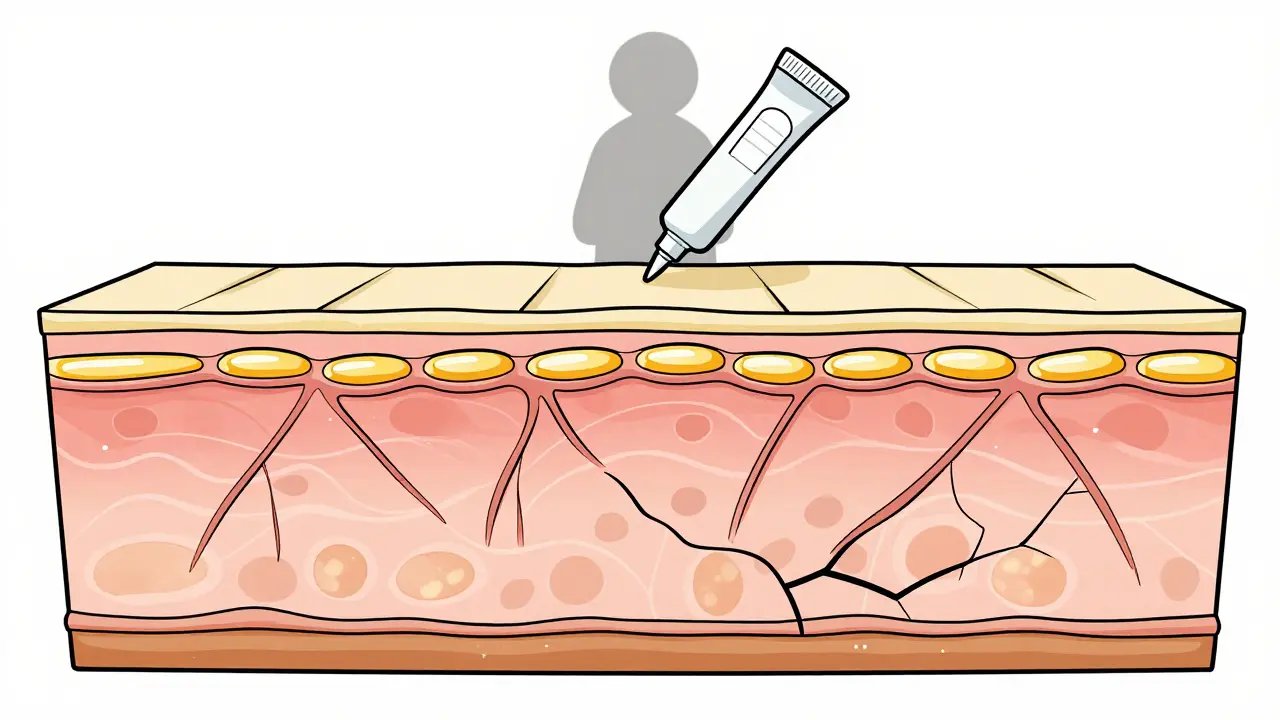
How Topical Steroids Thin Your Skin
Topical corticosteroids work by turning down inflammation, but they don’t just target the bad cells. They also shut down the skin’s natural repair system. The epidermis-the outer layer of skin-starts to thin because keratinocytes, the cells that rebuild your skin barrier, stop multiplying. At the same time, fibroblasts in the dermis stop making collagen, the protein that gives skin its strength and bounce. This isn’t just surface-level thinning. It’s structural damage.
Studies show that even three days of using a potent steroid cream can reduce collagen production. Over time, this leads to visible changes: skin that looks translucent, fine lines that don’t fade (called "elephant wrinkles"), and stretch marks (striae) that won’t go away. The skin becomes fragile-easily bruised, torn, or irritated by things that used to be harmless, like a cotton shirt or a light breeze.
The real problem? The damage isn’t always obvious right away. The surface might look fine, but underneath, the barrier is breaking down. Ceramides, cholesterol, and fatty acids-the lipids that seal in moisture and keep out irritants-drop by up to 60% in long-term users. This means your skin can’t hold water. It loses elasticity. And it becomes a doorway for bacteria and fungi.
The Infection Risk You Can’t Ignore
Thinner skin means less protection. When the skin barrier is weakened by steroids, it’s no longer a wall-it’s a sieve. That’s when infections start. Fungal infections like candidiasis (yeast) are common in moist areas like the armpits, groin, or under the breasts. Bacterial infections, especially from Staphylococcus aureus, can flare up as red, oozing patches that don’t respond to regular antibiotics because they’re hiding under the steroid’s anti-inflammatory mask.
One of the most misleading signs is "rebound redness." A patient stops using their steroid cream, thinking they’re healed, only to see the rash come back worse than before. That’s not a relapse of the original condition. It’s an infection taking advantage of the damaged barrier. Many doctors mistake this for steroid-resistant eczema. It’s not. It’s a broken skin barrier begging for help, not more steroids.
Perioral dermatitis-small red bumps around the mouth-is another classic sign. It’s often triggered by steroid creams applied to the face. Once the cream stops, the rash doesn’t just fade. It flares, sometimes for months. And if you keep applying more steroid to calm it? You’re just digging the hole deeper.
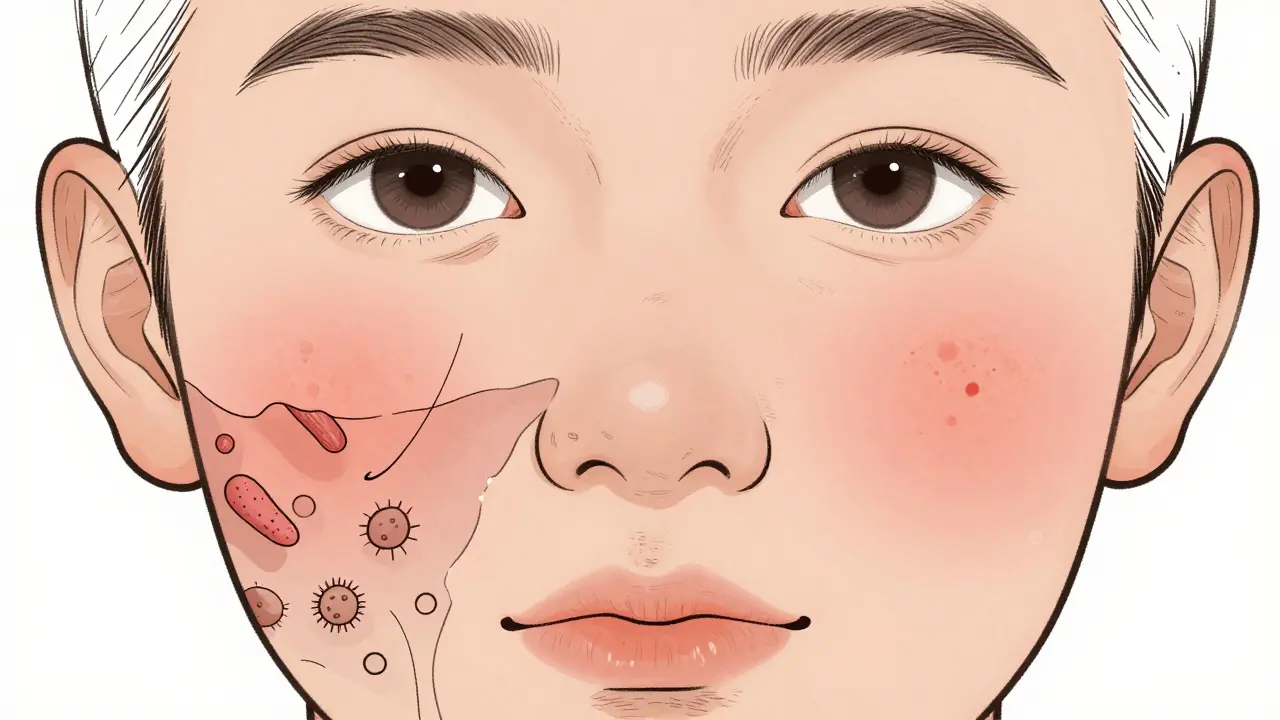
Who’s at Highest Risk?
Not everyone who uses topical steroids gets skin atrophy. But some people are far more vulnerable.
- Children: Their skin is 3 to 5 times thinner than adults’. Even mild steroids can cause damage if used daily for more than a few weeks.
- Face, eyelids, neck, and skin folds: These areas absorb steroids faster. Using strong creams here is like applying a chemical peel daily.
- Long-term users: Using a potent steroid (Class I-IV) for more than two weeks straight increases atrophy risk by 17%. For those using them for months or years, the chance of permanent stretch marks jumps to over 7%.
- People with sun exposure: UV rays break down collagen. Steroids do too. Together, they accelerate damage. A 2004 study found that unprotected skin on steroid-treated areas lost 42% more collagen than protected skin.
And here’s something most people don’t know: inhaled corticosteroids (used for asthma) can also cause skin atrophy. A Medsafe study in 2004 showed that even low daily doses (200-800 mcg) reduced collagen precursors in the skin after just six weeks. That’s right-breathing in steroids can thin your skin.
What Happens When You Stop
Stopping topical steroids isn’t as simple as just quitting. If you’ve used a potent cream for more than two weeks, stopping suddenly can trigger a severe reaction called Topical Steroid Withdrawal (TSW). Symptoms include:
- Intense burning or stinging, often worse than the original rash
- Red, flaky, oozing skin
- Hair loss in affected areas
- Swelling and tightness
- Insomnia and anxiety
The timeline is brutal. A 2014 NIH review of 127 patients found that the first flare starts about a week after stopping, lasts two weeks, then fades. But within another two weeks, a second, stronger flare hits. This cycle repeats-each flare shorter, but the recovery longer. The more years you used steroids, the longer the withdrawal lasts. One Reddit community of nearly 4,300 users reported an average recovery time of 8.2 months-with some taking over two years.
And it’s not just physical. Many patients describe feeling like they’ve lost their skin identity. They can’t wear makeup. They avoid mirrors. They feel isolated. This isn’t "just a rash." It’s a trauma to the skin’s entire ecosystem.
How to Prevent and Reverse the Damage
The good news? Skin can heal-but only if you stop the steroid and give it the right tools.
Prevention is simple:
- Use the lowest strength that works. Never use Class I-IV steroids on the face unless directed by a dermatologist.
- Limit use to 7-14 days on sensitive areas. Never apply more than twice daily.
- Avoid using steroids on broken or infected skin. That’s when damage spreads fastest.
- Always use sunscreen. SPF 50+ reduces collagen loss by 42% in atrophic skin.
Recovery requires a three-step plan:
- Stop or taper: If you’ve used a strong steroid for over two weeks, don’t quit cold turkey. Work with a doctor to reduce frequency slowly-cutting from twice daily to once daily, then every other day-over several weeks.
- Repair the barrier: Use creams with ceramides, cholesterol, and free fatty acids in a 3:1:1 ratio. A 2020 trial showed 68.4% improvement in barrier function after eight weeks. Look for products labeled "barrier repair" or "ECM support."
- Protect and wait: Avoid hot showers, harsh soaps, and fragrances. Let the skin rebuild naturally. It takes time. Patience isn’t optional-it’s the treatment.
There’s no magic cream that fixes steroid damage overnight. But your skin remembers how to heal. It just needs the right conditions.
The Future: Safer Alternatives
Pharma companies are finally listening. New "dual-soft" glucocorticoid agonists are in development-drugs that reduce inflammation without blocking collagen. Early trials show promise. The NIH is testing a topical formula that combines low-dose steroids with fibroblast growth factor to rebuild skin structure. Early results show a 63% drop in atrophy compared to standard treatment.
Meanwhile, the global market for steroid-sparing treatments is expected to hit $3.8 billion by 2028. That’s not just business-it’s proof that patients are demanding safer options.
Topical corticosteroids aren’t evil. They’re powerful tools. But like any tool, they’re dangerous in the wrong hands-or the wrong skin. The key isn’t to avoid them entirely. It’s to use them with respect: short-term, low-dose, and always with a plan to stop.
Can skin atrophy from topical steroids be reversed?
Yes, but only if caught early. Mild thinning and barrier damage can improve within 3-6 months after stopping steroids and using barrier-repair creams. However, once stretch marks (striae) form or collagen is permanently degraded, the damage is irreversible. Early intervention is critical.
Are over-the-counter steroid creams safe?
Not always. Many OTC creams contain hydrocortisone 1% or stronger, often labeled as "for itching" or "for rashes." Used daily for more than two weeks, even these can cause atrophy, especially on the face or in children. Always check the active ingredient and avoid long-term use without medical advice.
Why do some doctors still recommend long-term steroid use?
Many doctors were trained to treat flare-ups with steroids as a first-line response, without full awareness of long-term risks. Guidelines from the American Academy of Dermatology now clearly state that potent steroids should be limited to 2-4 weeks on sensitive areas. But outdated practices still exist, especially in areas with limited access to dermatologists. Patients should ask: "What’s my exit plan?" before starting.
Is topical steroid withdrawal real, or just anecdotal?
It’s real-and medically recognized. The NIH, European Medicines Agency, and Medsafe (New Zealand) all acknowledge TSW as a clinical phenomenon. Studies tracking 127+ patients show a consistent pattern of rebound inflammation, burning, and skin shedding after steroid cessation. The symptoms match known biological mechanisms: immune rebound, barrier collapse, and cytokine surges. It’s not "in your head." It’s your skin fighting back.
What’s the best cream to use after stopping steroids?
Look for products with a 3:1:1 ratio of ceramides, cholesterol, and free fatty acids. These are the exact lipids your skin loses. Brands like CeraVe, Avene Cicalfate, and EpiCeram have been clinically tested. Avoid anything with alcohol, fragrance, or essential oils-they irritate damaged skin. Apply twice daily, even if the skin looks fine. Healing happens underneath.
Can I use moisturizers while on steroids?
Yes-but not right before or after applying steroids. Moisturizers can increase steroid absorption. Wait at least 30 minutes after steroid application before moisturizing. Or, use moisturizers on non-treated days. The goal is to keep the skin hydrated without amplifying steroid penetration.
Topical corticosteroids saved millions from unbearable rashes. But they also left a trail of damaged skin. The lesson isn’t to fear them-it’s to use them wisely. Short. Rare. With eyes wide open.